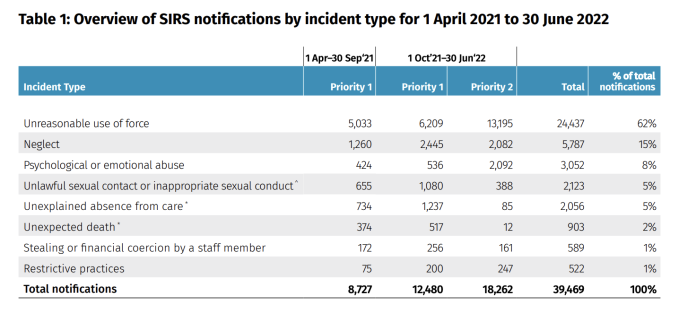
The Aged Care Quality and Safety Commission has released a report featuring case studies to provide insights and guidance to providers and staff in managing and preventing unreasonable use of force in residential aged care. The report is based on the Serious Incident Response Scheme (SIRS) ‘unreasonable use of force’ incident notifications that accounted for almost two-thirds of all incidents reported to the Commission by residential aged care providers between 1 April 2021 and 30 June 2022.
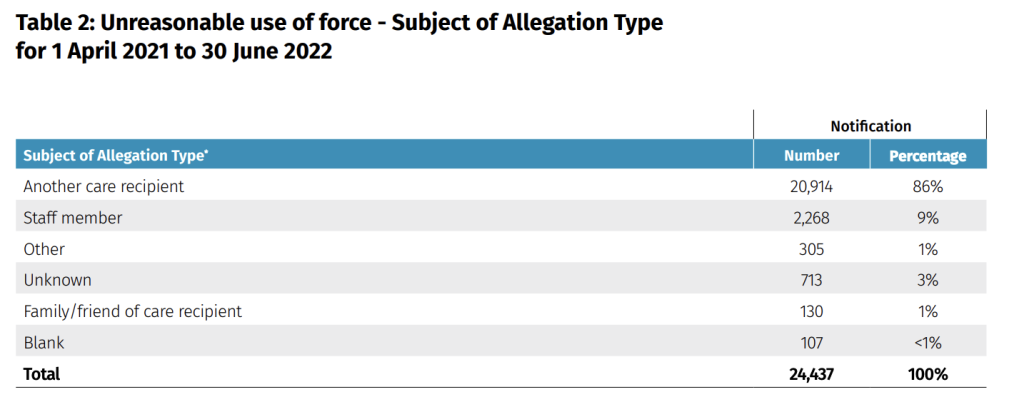
The report highlights that more than 86% of unreasonable use of force incidents involved interactions between residents, and more than 60% of residents were using unreasonable force. The affected residents were mostly reported to have severe cognitive impairment. The report recognises the challenges of preventing and managing these incidents but emphasises that many of them are avoidable, and providers must identify and mitigate risks to consumers in their service.
The SIRS was introduced for residential aged care services in April 2021 and was expanded on 1 December 2022 to include home care and flexible care, bringing greater visibility to serious incidents in aged care. Under the scheme, aged care providers must notify the Commission of serious incidents impacting consumers, have an effective incident management system, and identify how they understand, respond to, and learn from serious incidents when they occur.
Aged Care Quality and Safety Commissioner Janet Anderson said that the SIRS notifications give the Commission another way to understand how effectively individual providers are managing risks in aged care, and the notifications serve as additional intelligence about provider performance that, when combined with other Commission data, assists the Commission to better identify and respond to provider and service level risk.
The Commission uses the SIRS data to shape their education, information and guidance products to help consumers learn about common risks that can impact the quality and safety of care and to ask providers how they are managing these risks. For providers, the resources offer an opportunity to examine and benchmark their service’s performance and to take any actions to reduce the risk of, and/or improve their response to, serious incidents.
Ms Anderson said that reducing the chance of a serious incident occurring requires providers to identify, manage and mitigate risks to consumers, learn from every incident, and introduce preventative measures to avoid any recurrence. The Commission expects to see improvements in providers’ identification and response to incidents, including more careful analysis and better recording and reporting, as providers’ ability to manage incidents improves.
The report highlights that the number of serious incident notifications does not necessarily relate to the number of instances of harm to an aged care recipient, and reports can include multiple notifications about the same matter, suspected incidents, and situations where incidents occurred, but injury was avoided.
The Commission expressed concern about the aspect of managing incidents where some providers still need to improve at an operational and governance level. For instance, the Commission is concerned that nine out of ten providers are assessing incidents involving unreasonable use of force as having minor or no impact. It is possible that they are not considering less obvious impacts, which may be harder to identify where a resident is unable to reliably relate what happened, or delayed impacts where a physical injury becomes apparent later.
The report recommends that providers and their staff should use case studies as a learning tool to reflect on incidents at their own services and make changes that can reduce the chance of incidents recurring. Dr Melanie Wroth, the Commission’s Chief Clinical Advisor, said that providers who are genuinely interested in improving things for those in their care can deliver a better experience for every resident, irrespective of their level of cognitive impairment.